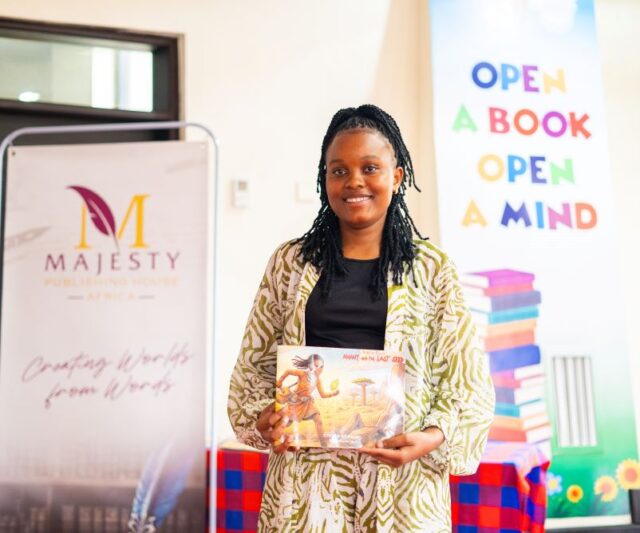‘Amani and the Last Seed’ -how one Kenyan author is teaching kids about climate action
By Maryanne W. Waweru l maryanne@mummytales.com
At just 25, Cynthia Wambua is already telling stories that matter. A communication specialist and filmmaker, Cynthia is now adding the title of ‘children’s author’ to her growing list of accomplishments with her debut book Amani and the Last Seed. Driven by a deep passion for environmental conservation and authentic African storytelling, Cynthia is on a mission to raise a generation of children who see themselves as part of the solution to the world around them.
Amani and the Last Seed, a Kenyan children’s book targeting ages 4 – 10 years, introduces readers to Amani, a brave, thoughtful girl who takes action to protect her environment. Through this story, children learn that even the smallest of actions can make a big difference.
Launched on Saturday 25 April 2026, the book is available at Nuria Bookstore and through Majesty Publishing House Africa, its publisher. You can also order a copy directly from the author on +254 715 794 586.
In this interview with Mummy Tales, Cynthia shares the inspiration behind her first book, why representation matters in children’s literature, and how parents can nurture a love for reading in their children while raising little changemakers along the way.
Maryanne: Briefly tell us what Amani and the Last Seed is about.
Cynthia: Amani and the Last Seed tells the story of a young girl living in the village of Kidani, who stumbles upon what may be the last remaining seed. Through this seed, Amani takes it upon herself to restore her village which has been harshly affected by climate change. Her actions demonstrate how one small act can lead to transformation.
Maryanne: What inspired you to write Amani and the Last Seed, especially as your first published book?
Cynthia: I was inspired to write Amani and the Last Seed because I wanted to tell the story of Wangari Maathai through her lens as a hero. I am also deeply passionate about nature and environmental conservation, so it felt like the perfect story to begin with.
Maryanne: Why did you choose environmental conservation as the central theme for a children’s story?
Cynthia: I love nature, especially the importance of taking care of trees and our environment. It’s something I want to instil in the younger generation, for them to understand that the power to protect and preserve the environment is in their hands.
Maryanne: Amani is portrayed as a young girl taking initiative. What message were you hoping children would take from her journey?
Cynthia: I want children to see themselves as the heroes this world needs for change to happen. It’s not just an adult’s responsibility -that they too can take the lead in creating positive change in society.
Maryanne: How important was it for you to create a strong African child as the main character in your story?
Cynthia: Growing up, most of the stories I read featured white characters as the heroes. I rarely saw African characters portrayed as powerful or heroic. My writing was an intentional move to change that narrative and to show that an African child can also be a hero, and to give society a chance to read stories about us, written by us. That is why my book features a young African child as the hero.

Maryanne: What does ‘authentic African storytelling’ in children’s literature mean to you?
Cynthia: It means telling stories that come from within us, stories rooted in our culture, experiences and identity, and as told by Africans.
Maryanne: What role do you think parents play in nurturing a love for reading?
Cynthia: Parents play a leading role. Reading should not feel like an academic task, but as a fun way to spend time together, just like in the old times when grandparents would share stories by the fireside about old legends.
Maryanne: What conversations do you hope this book will spark between parents and their children?
Cynthia: I hope that this book will remind children to believe in themselves and that nothing is impossible. I also hope it encourages parents to reassure their children that they are not too small or young to dream big and make a change.
Maryanne: How can African parents encourage their children to connect more with locally relevant stories?
Cynthia: They can:
- Make local stories part of daily life
- Buy and support African-authored books
- Use storytelling as a bonding activity
- Encourage children to tell and recreate stories they hear and read
Maryanne: What are some simple ways Kenyan mums can inculcate a reading culture in their homes?
Cynthia: They can make reading a normal and enjoyable part of everyday life. Most importantly, they can be a visible reading role model since children learn a lot from what they see.
Maryanne: What was the most challenging part of writing your first book?
Cynthia: I intend to have this as a series of African heroes, and so choosing the hero who will take the lead for others was a bit challenging, as we have many African heroes whose stories are yet to be told. Finding the publishing house that understands and carries the vision of telling African stories was also challenging, but I was gIad to have found Majesty Publishing House Africa who carried the vision.
Maryanne: From idea to publication. How long did that journey take?
Cynthia: It took almost two years. This is because it is something I wanted to be strategic about and needed to have a sense of direction of the why and what matters most. So even after I got the idea to write about our heroes, I needed all the support I could get to bring my idea to life, and this took quite some time. I was, however, glad to get the right people to work with.
Maryanne: What has the response been like since the book’s launch?
Cynthia: The response has been so great, and the book has been received positively, making a lot of sales despite it being just two weeks old in the market. I am truly grateful. One parent even shared that her son, who attended the launch and got a copy, was inspired and just begun writing -his point of reference being my book.
Maryanne: Are there plans to expand Amani’s story into a series or other formats?
Cynthia: Yes! The book is currently being adapted into an animation, and I am also preparing the next story featuring another African hero. This will be part of a series highlighting different African heroes. That’s what’s next for me.
Thanks Cynthia and all the best.
So that was my converstion with Cynthia. As a mum and a storyteller myself, I truly believe that the books we place in our children’s hands matter. Amani and the Last Seed is one of those stories worth sharing. I encourage you to get a copy, not just for your child, but for the both of you. Read it together. Talk about it. You might be surprised by how much they already understand, and how eager they are to create change around them.
Are you a woman Kenyan author? If you would you like to featured on the Mummy Tales blog, send an email with a brief introduction about yourself and your book to maryanne@mummytales.com
Also read:‘Deportee’ by Wanjiku Gitagia: book review & interview
Also read:‘Shadows in my Sunshine’ by Beth Ruga: book review & interview
Also read: ‘The Strength we Share’ by Diana A. Otieno book review & interview
Also read:‘Risking it All’ by Anna-Maria Mwachinga book review
 Mummy Tales by Maryanne W. Waweru is a platform dedicated to empowering its readers on different aspects of womanhood and motherhood. Read more motherhood experiences of Kenyan moms here. Connect with Mummy Tales on: FACEBOOK l YOU TUBE l TWITTER
Mummy Tales by Maryanne W. Waweru is a platform dedicated to empowering its readers on different aspects of womanhood and motherhood. Read more motherhood experiences of Kenyan moms here. Connect with Mummy Tales on: FACEBOOK l YOU TUBE l TWITTER